Expo
view channel
view channel
view channel
view channel
view channel
view channel
view channel
view channel
view channel
Clinical Chem.Molecular DiagnosticsHematologyImmunologyMicrobiology
TechnologyIndustry
Events
Webinars

- Liquid Biopsy Biomarkers May Improve Childhood Epilepsy Diagnosis
- Blood-Based Sensor Detects Early Signs of Alzheimer’s and Parkinson’s
- Urine-Based Alzheimer’s Test Receives FDA Breakthrough Device Designation
- Fluid Biomarker Improves Diagnosis and Monitoring of Primary CNS Lymphoma
- New CA19-9 Cutoff Value Helps Identify High-Risk Pancreatic Cancer Patients
- Digital PCR Assays Support Surveillance of Bundibugyo Ebolavirus Outbreak
- Blood-Based Proteomic Test May Predict Treatment Response in Non-Small Cell Lung Cancer
- Ultrasensitive MRD Blood Test Detects Early Breast Cancer Recurrence
- Position Statements Outline Evidence Standards for Multi-Cancer Detection Tests
- Gene Fusion Patterns May Flag High Risk Solitary Fibrous Tumors
- Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
- Higher Ferritin Threshold May Improve Iron Deficiency Detection in Children
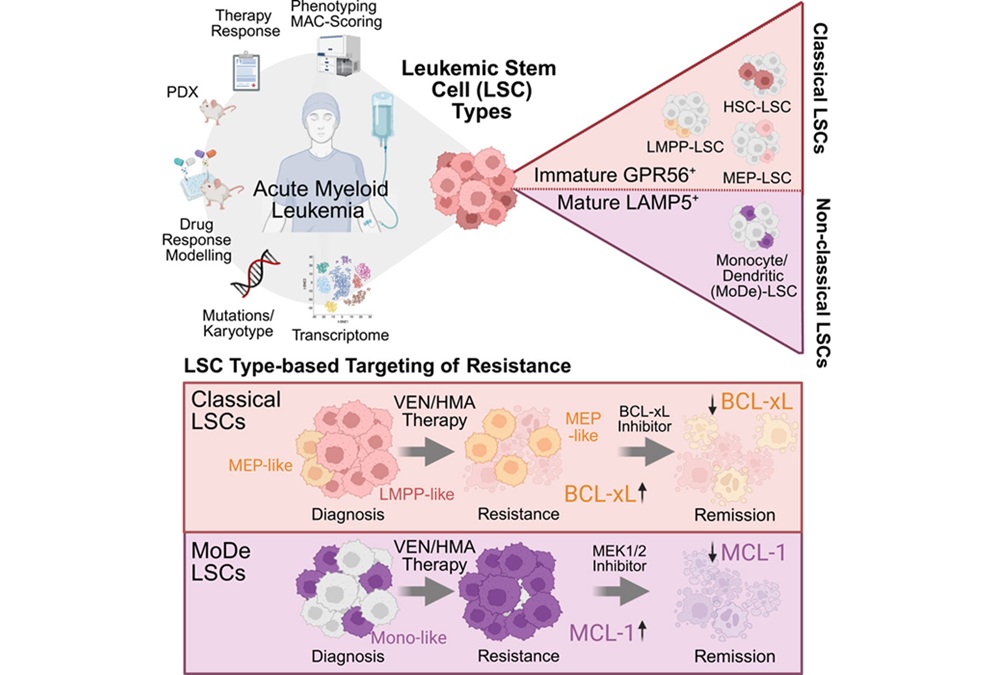
- Stem Cell Biomarkers May Guide Precision Treatment in Acute Myeloid Leukemia
- Advanced CBC-Derived Indices Integrated into Hematology Platforms
- Blood Test Enables Early Detection of Multiple Myeloma Relapse
- Immune Enzyme Linked to Treatment-Resistant Inflammatory Bowel Disease
- Simple Blood Test Could Replace Biopsies for Lung Transplant Rejection Monitoring
- Routine TB Screening Test May Reveal Immune Aging and Mortality Risk
- Biomarkers and Molecular Testing Advance Precision Allergy Care
- Point-of-Care Tests Could Expand Access to Mpox Diagnosis
- FDA-Cleared Gastrointestinal Panel Detects 24 Pathogen Targets
- New AMR Assay Supports Rapid Infection Control Screening in Hospitals
- Diagnostic Gaps Complicate Bundibugyo Ebola Outbreak Response in Congo
- Study Finds Hidden Mpox Infections May Drive Ongoing Spread
- Large-Scale Genomic Surveillance Tracks Resistant Bacteria Across European Hospitals
- Algorithm Panel Aids Liver Fibrosis Assessment and Liver Cancer Surveillance
- AI-Enabled Assistant Unifies Molecular Workflow Planning and Support
- AI Tool Automates Validation of Laboratory Software Configuration Changes
- Point-of-Care Testing Enhances Health Literacy and Self-Management in Chronic Disease
- Fully Automated Sample-to-Insight Workflow Advances Latent TB Testing
- ClearNote Health to Present Pancreatic Cancer Blood Test Data at ASCO 2026
- New Distribution Agreement Expands Access to CE-Marked Precision Oncology Assays
- Artera to Highlight AI-Based Cancer Risk Stratification at ASCO 2026
- Natera to Present Data on MRD-Guided Cancer Care at ASCO 2026
- Fujifilm Integrates Structured Reporting into Digital Pathology Workflow
- Tumor Genome Marker May Predict Treatment Benefit in Pediatric Cancers
- Lysosomal Gene Defect Linked to Severe Childhood Brain Disorders
- Genetic Testing Identifies Greater Inherited Sudden Cardiac Arrest Risk in Younger Individuals
- Hidden 'Jumping Gene' Variant Linked to Higher Pancreatic Cancer Risk
- Common White Blood Cells Produce Schizophrenia-Linked Protein
- AI Tool Extracts Immune Signals from Biopsy to Inform Myeloma Therapy
- Rapid AI Tool Predicts Cancer Spatial Gene Expression from Pathology Images
- AI Pathology Test Receives FDA Breakthrough for Bladder Cancer Risk Stratification
- FDA Clears AI Digital Pathology Tool for Breast Cancer Risk Stratification
- New AI Tool Reveals Hidden Genetic Signals in Routine H&E Slides

 Expo
Expo
- Liquid Biopsy Biomarkers May Improve Childhood Epilepsy Diagnosis
- Blood-Based Sensor Detects Early Signs of Alzheimer’s and Parkinson’s
- Urine-Based Alzheimer’s Test Receives FDA Breakthrough Device Designation
- Fluid Biomarker Improves Diagnosis and Monitoring of Primary CNS Lymphoma
- New CA19-9 Cutoff Value Helps Identify High-Risk Pancreatic Cancer Patients
- Digital PCR Assays Support Surveillance of Bundibugyo Ebolavirus Outbreak
- Blood-Based Proteomic Test May Predict Treatment Response in Non-Small Cell Lung Cancer
- Ultrasensitive MRD Blood Test Detects Early Breast Cancer Recurrence
- Position Statements Outline Evidence Standards for Multi-Cancer Detection Tests
- Gene Fusion Patterns May Flag High Risk Solitary Fibrous Tumors
- Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
- Higher Ferritin Threshold May Improve Iron Deficiency Detection in Children
- Stem Cell Biomarkers May Guide Precision Treatment in Acute Myeloid Leukemia
- Advanced CBC-Derived Indices Integrated into Hematology Platforms
- Blood Test Enables Early Detection of Multiple Myeloma Relapse
- Immune Enzyme Linked to Treatment-Resistant Inflammatory Bowel Disease
- Simple Blood Test Could Replace Biopsies for Lung Transplant Rejection Monitoring
- Routine TB Screening Test May Reveal Immune Aging and Mortality Risk
- Biomarkers and Molecular Testing Advance Precision Allergy Care
- Point-of-Care Tests Could Expand Access to Mpox Diagnosis
- FDA-Cleared Gastrointestinal Panel Detects 24 Pathogen Targets
- New AMR Assay Supports Rapid Infection Control Screening in Hospitals
- Diagnostic Gaps Complicate Bundibugyo Ebola Outbreak Response in Congo
- Study Finds Hidden Mpox Infections May Drive Ongoing Spread
- Large-Scale Genomic Surveillance Tracks Resistant Bacteria Across European Hospitals
- Algorithm Panel Aids Liver Fibrosis Assessment and Liver Cancer Surveillance
- AI-Enabled Assistant Unifies Molecular Workflow Planning and Support
- AI Tool Automates Validation of Laboratory Software Configuration Changes
- Point-of-Care Testing Enhances Health Literacy and Self-Management in Chronic Disease
- Fully Automated Sample-to-Insight Workflow Advances Latent TB Testing
- ClearNote Health to Present Pancreatic Cancer Blood Test Data at ASCO 2026
- New Distribution Agreement Expands Access to CE-Marked Precision Oncology Assays
- Artera to Highlight AI-Based Cancer Risk Stratification at ASCO 2026
- Natera to Present Data on MRD-Guided Cancer Care at ASCO 2026
- Fujifilm Integrates Structured Reporting into Digital Pathology Workflow
- Tumor Genome Marker May Predict Treatment Benefit in Pediatric Cancers
- Lysosomal Gene Defect Linked to Severe Childhood Brain Disorders
- Genetic Testing Identifies Greater Inherited Sudden Cardiac Arrest Risk in Younger Individuals
- Hidden 'Jumping Gene' Variant Linked to Higher Pancreatic Cancer Risk
- Common White Blood Cells Produce Schizophrenia-Linked Protein
- AI Tool Extracts Immune Signals from Biopsy to Inform Myeloma Therapy
- Rapid AI Tool Predicts Cancer Spatial Gene Expression from Pathology Images
- AI Pathology Test Receives FDA Breakthrough for Bladder Cancer Risk Stratification
- FDA Clears AI Digital Pathology Tool for Breast Cancer Risk Stratification
- New AI Tool Reveals Hidden Genetic Signals in Routine H&E Slides