Expo
view channel
view channel
view channel
view channel
view channel
view channel
view channel
view channel
view channel
Clinical Chem.
HematologyImmunologyMicrobiologyPathologyTechnologyIndustry
Events
Webinars

- Blood-Based Biomarkers Show Promise for Psychosis Risk Prediction
- International Experts Recommend Ending Routine 'Corrected' Calcium Reporting
- Long-Term Data Show PSA Screening Modestly Reduces Prostate Cancer Deaths
- Urine-Based Nanosensor Tracks Lung Cancer and Fibrosis Noninvasively
- Blood-Based Alzheimer’s Test Gains CE Mark for Amyloid Pathology Detection
- FDA Approves Expanded Liquid Biopsy Panel for Advanced Cancer Profiling
- Microbial Saliva Test Could Help Triage Esophageal Cancer Risk
- Expanded DPYD Genotyping Test Supports Safer Chemotherapy Dosing
- Multi-Omics Profiling Helps Predict BCG Response and Recurrence in Bladder Cancer
- New Computational Tool Reveals Genetic Driver of Idiopathic Neuropathy
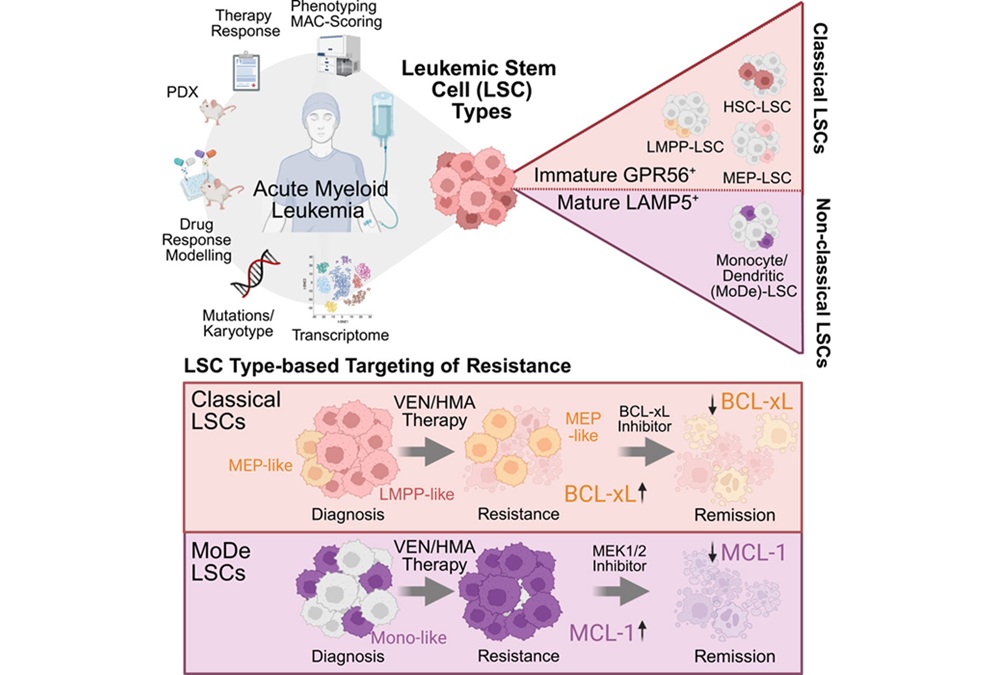
- Stem Cell Biomarkers May Guide Precision Treatment in Acute Myeloid Leukemia
- Advanced CBC-Derived Indices Integrated into Hematology Platforms
- Blood Test Enables Early Detection of Multiple Myeloma Relapse
- Single Assay Enables Rapid HLA and ABO Genotyping for Transplant Matching
- Prognostic Biomarker Identified in Diffuse Large B-Cell Lymphoma
- Simple Blood Test Could Replace Biopsies for Lung Transplant Rejection Monitoring
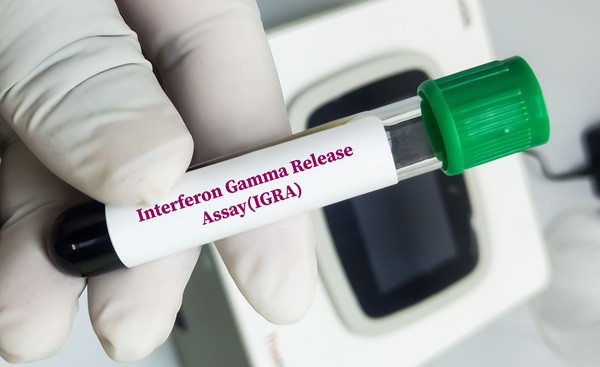
- Routine TB Screening Test May Reveal Immune Aging and Mortality Risk
- Biomarkers and Molecular Testing Advance Precision Allergy Care
- Point-of-Care Tests Could Expand Access to Mpox Diagnosis
- T-Cell Senescence Profiling May Predict CAR T Responses
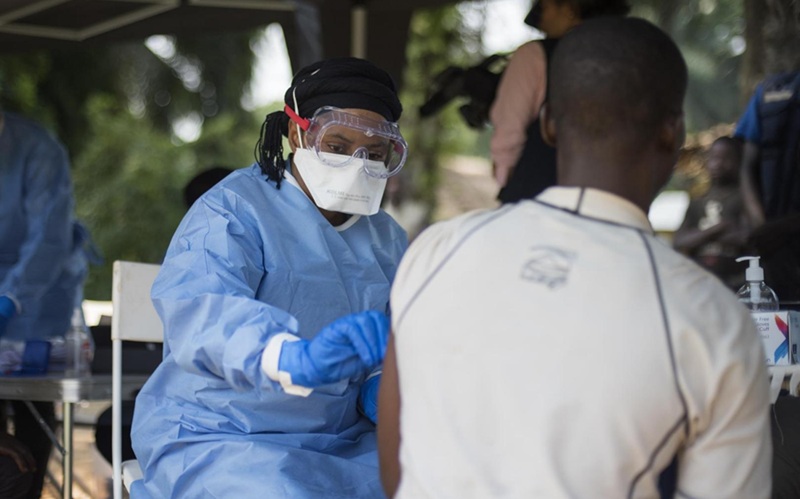
- Diagnostic Gaps Complicate Bundibugyo Ebola Outbreak Response in Congo
- Study Finds Hidden Mpox Infections May Drive Ongoing Spread
- Large-Scale Genomic Surveillance Tracks Resistant Bacteria Across European Hospitals
- Molecular Urine and Stool Tests Do Not Improve Early TB Treatment in Hospitalized HIV Patients
- Rapid Antigen Biosensor Detects Active Tuberculosis in One Hour
- AI Tool Automates Validation of Laboratory Software Configuration Changes
- Point-of-Care Testing Enhances Health Literacy and Self-Management in Chronic Disease
- Fully Automated Sample-to-Insight Workflow Advances Latent TB Testing
- Tumor-on-a-Chip Platform Models Pancreatic Cancer Treatment Response
- New Platform Captures Extracellular Vesicles for Early Cancer Detection
- Partnership Brings Single-Cell Analysis into Clinical Oncology Workflows
- AI-Powered Multi-Functional Analyzer Wins German Innovation Award
- Partnership Aims to Bring Risk-Guided CKD Care to Health Systems
- Roche to Acquire PathAI for Up to $1.05 Billion to Strengthen AI Diagnostics Portfolio
- FDA Clears Blood-Based Companion Diagnostic for Advanced Breast Cancer Therapy
- Hidden 'Jumping Gene' Variant Linked to Higher Pancreatic Cancer Risk
- Common White Blood Cells Produce Schizophrenia-Linked Protein
- Nanopore Method Captures RNA Folding at Single-Molecule Resolution
- Tumor Microenvironment Marker Linked to Worse Survival in Solid Tumors
- Genetic Markers May Help Predict Amputation Risk in Peripheral Artery Disease
- AI Pathology Test Receives FDA Breakthrough for Bladder Cancer Risk Stratification
- FDA Clears AI Digital Pathology Tool for Breast Cancer Risk Stratification
- New AI Tool Reveals Hidden Genetic Signals in Routine H&E Slides
- AI System Analyzes Routine Pathology Slides to Predict Cancer Outcomes
- New Tissue Mapping Approach Identifies High-Risk Form of Diabetic Kidney Disease

 Expo
Expo
- Blood-Based Biomarkers Show Promise for Psychosis Risk Prediction
- International Experts Recommend Ending Routine 'Corrected' Calcium Reporting
- Long-Term Data Show PSA Screening Modestly Reduces Prostate Cancer Deaths
- Urine-Based Nanosensor Tracks Lung Cancer and Fibrosis Noninvasively
- Blood-Based Alzheimer’s Test Gains CE Mark for Amyloid Pathology Detection
- FDA Approves Expanded Liquid Biopsy Panel for Advanced Cancer Profiling
- Microbial Saliva Test Could Help Triage Esophageal Cancer Risk
- Expanded DPYD Genotyping Test Supports Safer Chemotherapy Dosing
- Multi-Omics Profiling Helps Predict BCG Response and Recurrence in Bladder Cancer
- New Computational Tool Reveals Genetic Driver of Idiopathic Neuropathy
- Stem Cell Biomarkers May Guide Precision Treatment in Acute Myeloid Leukemia
- Advanced CBC-Derived Indices Integrated into Hematology Platforms
- Blood Test Enables Early Detection of Multiple Myeloma Relapse
- Single Assay Enables Rapid HLA and ABO Genotyping for Transplant Matching
- Prognostic Biomarker Identified in Diffuse Large B-Cell Lymphoma
- Simple Blood Test Could Replace Biopsies for Lung Transplant Rejection Monitoring
- Routine TB Screening Test May Reveal Immune Aging and Mortality Risk
- Biomarkers and Molecular Testing Advance Precision Allergy Care
- Point-of-Care Tests Could Expand Access to Mpox Diagnosis
- T-Cell Senescence Profiling May Predict CAR T Responses
- Diagnostic Gaps Complicate Bundibugyo Ebola Outbreak Response in Congo
- Study Finds Hidden Mpox Infections May Drive Ongoing Spread
- Large-Scale Genomic Surveillance Tracks Resistant Bacteria Across European Hospitals
- Molecular Urine and Stool Tests Do Not Improve Early TB Treatment in Hospitalized HIV Patients
- Rapid Antigen Biosensor Detects Active Tuberculosis in One Hour
- AI Tool Automates Validation of Laboratory Software Configuration Changes
- Point-of-Care Testing Enhances Health Literacy and Self-Management in Chronic Disease
- Fully Automated Sample-to-Insight Workflow Advances Latent TB Testing
- Tumor-on-a-Chip Platform Models Pancreatic Cancer Treatment Response
- New Platform Captures Extracellular Vesicles for Early Cancer Detection
- Partnership Brings Single-Cell Analysis into Clinical Oncology Workflows
- AI-Powered Multi-Functional Analyzer Wins German Innovation Award
- Partnership Aims to Bring Risk-Guided CKD Care to Health Systems
- Roche to Acquire PathAI for Up to $1.05 Billion to Strengthen AI Diagnostics Portfolio
- FDA Clears Blood-Based Companion Diagnostic for Advanced Breast Cancer Therapy
- Hidden 'Jumping Gene' Variant Linked to Higher Pancreatic Cancer Risk
- Common White Blood Cells Produce Schizophrenia-Linked Protein
- Nanopore Method Captures RNA Folding at Single-Molecule Resolution
- Tumor Microenvironment Marker Linked to Worse Survival in Solid Tumors
- Genetic Markers May Help Predict Amputation Risk in Peripheral Artery Disease
- AI Pathology Test Receives FDA Breakthrough for Bladder Cancer Risk Stratification
- FDA Clears AI Digital Pathology Tool for Breast Cancer Risk Stratification
- New AI Tool Reveals Hidden Genetic Signals in Routine H&E Slides
- AI System Analyzes Routine Pathology Slides to Predict Cancer Outcomes
- New Tissue Mapping Approach Identifies High-Risk Form of Diabetic Kidney Disease